You’ve probably felt it before — that sharp, shooting pain down your arm or leg that makes you wince. Maybe it’s a tingling sensation that won’t go away, or numbness that’s starting to worry you. Your first thought? “I must have a pinched nerve.” And while that might be true, sometimes what feels like a simple pinched nerve can actually be a sign of something more serious that needs immediate attention.
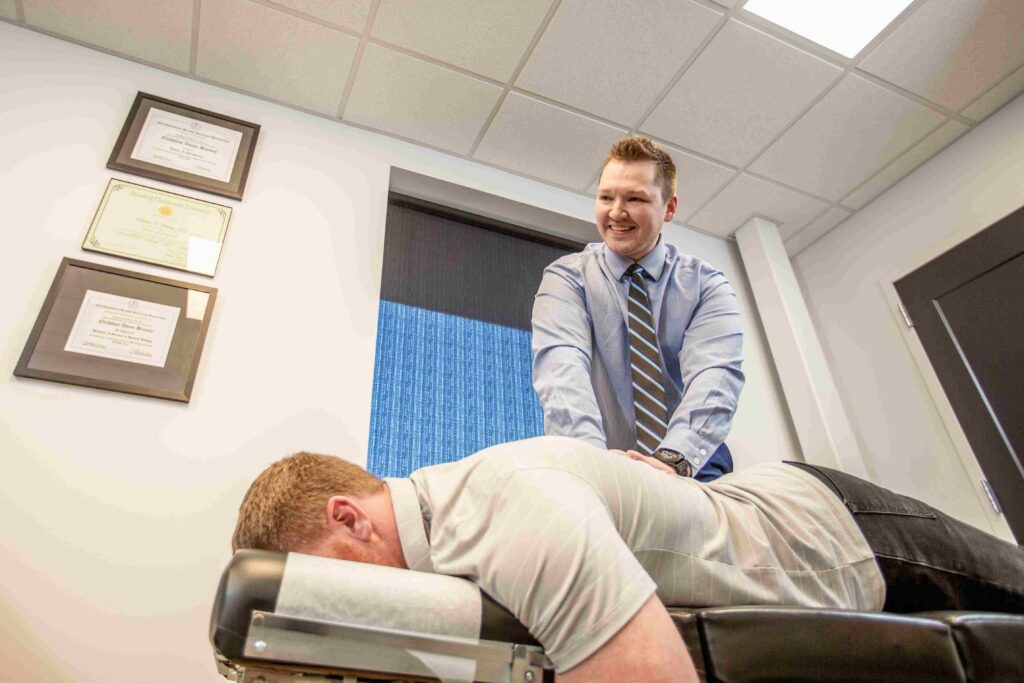
Here in West Fargo, we see patients every week at Optimal Chiropractic who’ve been dealing with nerve-related symptoms for weeks or even months, assuming it would just go away on its own. Understanding the difference between a straightforward nerve compression issue and something that requires urgent care can make all the difference in your recovery and long-term health.
What is a pinched nerve? A pinched nerve occurs when surrounding tissues — such as bones, cartilage, muscles, or tendons — apply too much pressure to a nerve root. This compression disrupts the nerve’s function, causing pain, tingling, numbness, or weakness in the affected area. While many pinched nerves respond well to conservative care, certain warning signs indicate a more serious underlying condition.
Table of Contents
- Understanding Nerve Compression: The Basics
- 5 Warning Signs Your Symptoms Need Immediate Attention
- Serious Conditions That Mimic Pinched Nerves
- How Chiropractic Evaluation Can Help Identify the Real Problem
- What You Should Do If You Notice These Warning Signs
- When to See a Chiropractor vs. When to Go to the ER
- Symptoms Comparison Table
- Myths vs. Facts About Nerve Pain
- Final Thoughts from Optimal Chiropractic
Understanding Nerve Compression: The Basics
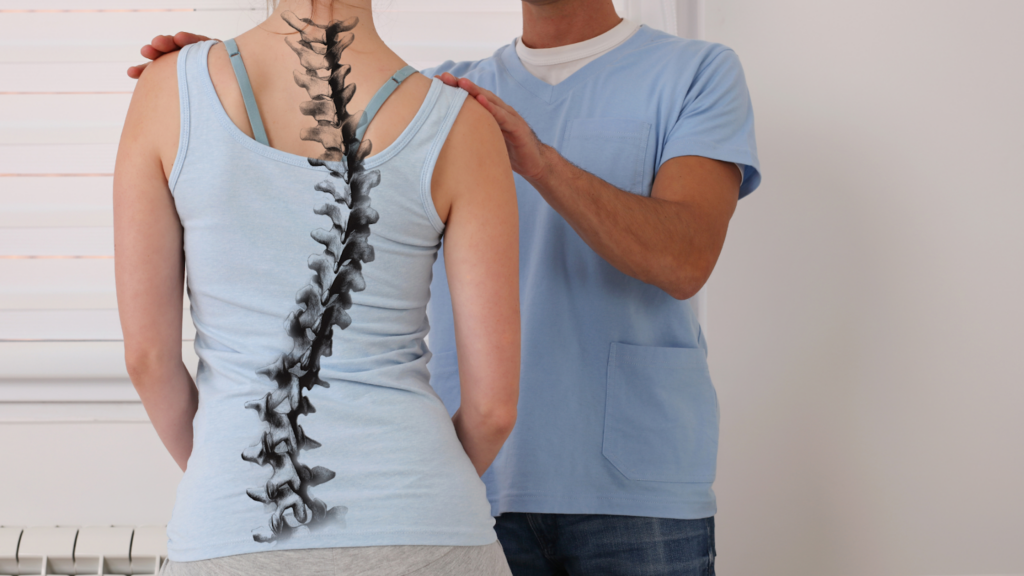
Before we dive into the warning signs, it’s helpful to understand what’s actually happening when a nerve gets compressed. Your nervous system is like an intricate highway system, with your brain and spinal cord serving as the main routes and peripheral nerves branching out to every part of your body.
When a nerve gets “pinched,” it means something is pressing on it. This could be a herniated disc, bone spur, inflamed muscle, or swollen tissue. The pressure interferes with the nerve’s ability to send signals properly, which is why you experience those uncomfortable symptoms like tingling, numbness, or radiating pain.
Most pinched nerves are relatively straightforward. They develop gradually from repetitive motions, poor posture, or minor injuries. With proper care — including chiropractic adjustments, rest, and lifestyle modifications — many people find relief within a few weeks.
However, certain symptoms suggest something more complex is happening. Your body has ways of telling you when a problem goes beyond simple nerve compression. Learning to recognize these signals can help you get the right care at the right time.
5 Warning Signs Your Symptoms Need Immediate Attention
Sign #1: Progressive Weakness That’s Getting Worse
A typical pinched nerve might cause some mild weakness in the affected area. You might notice your grip isn’t quite as strong, or your leg feels a bit wobbly. But if that weakness is progressively getting worse over days or weeks, that’s a red flag.
Progressive weakness suggests the nerve is experiencing significant or increasing compression. This could indicate a worsening disc herniation, spinal stenosis that’s advancing, or even a space-occupying lesion. At Optimal Chiropractic, when we see patients whose weakness has noticeably declined week over week, we take that very seriously.
Watch for signs like dropping objects frequently, difficulty walking up stairs when you could before, or being unable to perform tasks that were easy just last week. This isn’t the natural course of a simple pinched nerve, which typically stabilizes or improves with time and appropriate care.
Sign #2: Loss of Bowel or Bladder Control
This is perhaps the most serious warning sign on our list. Any loss of bowel or bladder control — or even changes in sensation in the groin or rectal area — requires immediate medical attention. This isn’t something to “wait and see” about.
These symptoms can indicate cauda equina syndrome, a rare but serious condition where the nerve roots at the lower end of the spinal cord are severely compressed. This is a medical emergency that requires immediate intervention, often surgical, to prevent permanent nerve damage.
Other symptoms that may accompany this include numbness in the saddle area (where you’d sit on a horse), severe lower back pain, and weakness in both legs. If you experience any of these symptoms, go to the emergency room immediately — don’t wait for an appointment.
Sign #3: Symptoms in Multiple Limbs or Both Sides of Your Body
A pinched nerve typically affects one side of your body. If you’re experiencing symptoms in your right arm, you usually won’t have them in your left arm too. So when symptoms appear on both sides simultaneously, or in multiple limbs at once, it suggests something more systemic is happening.
Bilateral symptoms (affecting both sides) could indicate spinal cord compression rather than a simple nerve root problem. Conditions like cervical or thoracic spinal stenosis, tumors, or certain neurological conditions can present this way. Multiple sclerosis, peripheral neuropathy, and other systemic neurological conditions may also cause widespread symptoms.
Here in West Fargo, we’ve had patients come to Optimal Chiropractic thinking they had multiple pinched nerves, when in reality, they needed a different type of evaluation. While chiropractic care can help with many musculoskeletal issues, some conditions require medical co-management or specialized testing.
Sign #4: Unexplained Fever, Weight Loss, or Night Sweats
Nerve pain accompanied by systemic symptoms like fever, unexplained weight loss, or drenching night sweats is not characteristic of a simple pinched nerve. These constitutional symptoms suggest your body is fighting something more significant.
Infections of the spine, such as discitis or osteomyelitis, can cause both nerve-type pain and fever. Certain cancers, whether primary spinal tumors or metastases from elsewhere, may present with nerve symptoms along with weight loss and night sweats. Autoimmune conditions affecting the nervous system can also produce this combination of symptoms.
Any time you have nerve symptoms plus these systemic warning signs, it warrants a thorough medical evaluation. Blood work, imaging, and sometimes specialized testing are necessary to identify the underlying cause. While these serious conditions are relatively rare, catching them early makes a significant difference in outcomes.
Sign #5: Severe Pain That’s Unrelieved by Position Changes or Rest
Most pinched nerve pain has a mechanical component. This means certain positions make it better or worse. You might notice that tilting your head a certain way eases neck pain and arm tingling, or that lying down provides some relief from sciatica.
When pain is severe and unrelenting — meaning nothing you do makes it better, not even temporarily — that’s concerning. Pain that wakes you from sleep and prevents you from finding any comfortable position may indicate something beyond simple nerve compression.
This type of pain pattern can be associated with fractures, infections, tumors, or severe disc herniations. It’s particularly worrying when combined with other symptoms on this list. The body usually gives you some relief with positional changes when dealing with mechanical issues, so constant, severe pain deserves prompt investigation.
Serious Conditions That Mimic Pinched Nerves
Understanding what else could be causing your symptoms helps explain why accurate diagnosis is so important. Several serious conditions can present with nerve-like symptoms that are easily mistaken for simple compression.
Spinal cord compression occurs when pressure is placed directly on the spinal cord itself, rather than just a nerve root. This can happen with severe disc herniations, spinal stenosis, tumors, or traumatic injuries. Symptoms often include weakness, coordination problems, and sometimes bowel or bladder changes. Unlike a pinched nerve, spinal cord issues affect larger areas of the body and can have more devastating consequences if left untreated.
Cauda equina syndrome, as mentioned earlier, is a medical emergency. The cauda equina is the bundle of nerve roots at the bottom of the spinal cord. When these become severely compressed, often from a large disc herniation, tumor, or trauma, it creates a constellation of serious symptoms requiring urgent surgical intervention.
Peripheral neuropathy describes nerve damage from various causes including diabetes, vitamin deficiencies, toxins, infections, or autoimmune diseases. The symptoms — numbness, tingling, burning sensations — can feel similar to a pinched nerve, but the underlying mechanism is completely different. This condition requires medical management of the underlying cause.
Spinal infections like discitis, osteomyelitis, or epidural abscess can create nerve-type pain along with systemic symptoms. These bacterial or fungal infections require antibiotic treatment and sometimes surgical drainage. They’re rare but serious, particularly in people with compromised immune systems.
Tumors — whether primary spinal tumors or metastases from cancers elsewhere — can compress nerves or the spinal cord. They often cause progressive symptoms that worsen over time, along with constitutional symptoms. Early detection through imaging is crucial for treatment planning.
At Optimal Chiropractic in West Fargo, part of our comprehensive evaluation includes screening for these red flags. When we identify concerning symptoms, we don’t hesitate to refer for advanced imaging or medical co-management. Your safety always comes first.
How Chiropractic Evaluation Can Help Identify the Real Problem
A thorough chiropractic examination involves much more than just looking at your spine. When you come to Optimal Chiropractic with nerve symptoms, we conduct a systematic evaluation designed to understand exactly what’s happening and whether your symptoms fit the pattern of a straightforward mechanical issue or something requiring additional investigation.
The evaluation begins with a detailed history. We ask about when symptoms started, what makes them better or worse, whether they’re improving or worsening, and whether you’ve experienced any of those red flag symptoms. This conversation often reveals important clues about the underlying cause.
Next comes orthopedic and neurological testing. We assess reflexes, muscle strength, sensation, and coordination. We perform specific tests to identify which nerve roots might be affected. Range of motion testing shows us how your spine moves and where restrictions exist. Palpation helps us identify areas of muscle tension, spinal misalignment, or inflammation.
Special tests help differentiate between different types of nerve problems. For example, tests like the straight leg raise can indicate disc herniation, while other maneuvers help identify peripheral nerve entrapment. We’re looking for patterns that match common chiropractic conditions versus those that suggest something outside our scope.
When findings suggest a straightforward mechanical problem — perhaps a facet joint issue, disc bulge, or muscle-related nerve irritation — we can often begin conservative chiropractic care with confidence. Techniques like spinal adjustments, soft tissue work, therapeutic exercises, and lifestyle modifications frequently provide excellent results for these conditions.
However, when red flags appear during our examination, we take a different approach. We may recommend imaging studies like X-rays or MRI before beginning treatment. We might refer you to your primary care physician for blood work or other medical evaluation. In some cases, we’ll coordinate care with other healthcare providers to ensure you’re getting comprehensive attention.
Research from organizations like the American Chiropractic Association emphasizes the importance of this screening role. Chiropractors are trained to recognize when symptoms fit patterns of common musculoskeletal problems and when they suggest something more serious. This gatekeeper function protects patients and ensures appropriate, timely care.
What You Should Do If You Notice These Warning Signs
If you recognize any of the five warning signs in yourself or a loved one, taking appropriate action quickly is important. Here’s a practical guide to help you respond appropriately based on your symptoms.
For loss of bowel or bladder control or symptoms suggesting cauda equina syndrome, go to the emergency room immediately. Don’t wait for an appointment. Don’t try home remedies first. This is a true medical emergency where hours matter. Call 911 if you’re unable to transport yourself safely.
For progressive weakness that’s clearly worsening week over week, schedule an urgent evaluation. Contact your chiropractor or primary care physician within a day or two, not weeks. Explain that your symptoms are progressively declining. Most offices, including Optimal Chiropractic, will prioritize patients with worsening neurological symptoms.
For bilateral symptoms or symptoms in multiple limbs, seek evaluation within a few days. While this may not require emergency room care, it does warrant relatively prompt attention. Be prepared for your provider to recommend imaging studies or referral for additional testing.
For nerve symptoms accompanied by fever, weight loss, or night sweats, contact your primary care physician or visit an urgent care center. These systemic symptoms combined with nerve pain require medical evaluation including blood work and likely imaging. Your doctor may refer you to a specialist depending on what initial tests reveal.
For severe, unrelenting pain that’s not responding to position changes or over-the-counter pain relievers, seek evaluation within a day or two. Document what you’ve tried and what hasn’t helped. This information helps your healthcare provider understand the severity and character of your symptoms.
In all cases, be your own advocate. If something feels seriously wrong, trust that instinct. It’s always better to have symptoms evaluated and find out they’re not serious than to delay evaluation of something that needs urgent attention. Healthcare providers would much rather see you sooner and reassure you than have you wait until a problem becomes more difficult to treat.
When to See a Chiropractor vs. When to Go to the ER
Understanding the appropriate level of care for your symptoms can be confusing. Here’s a practical framework to help you decide whether your nerve symptoms are appropriate for chiropractic evaluation or whether you need more urgent medical attention.
See a chiropractor when you have: Gradual onset of symptoms related to posture, movement, or minor injury. Pain that varies with position — some positions make it better, others worse. Symptoms limited to one side of your body or one specific nerve distribution. Mild to moderate symptoms that aren’t rapidly worsening. No red flag symptoms like those discussed earlier. Symptoms that seem related to mechanical or musculoskeletal issues.
Chiropractic care excels at addressing mechanical problems affecting the spine and nervous system. Research published in journals like Spine has shown that spinal manipulation can be effective for certain types of nerve-related pain, particularly when caused by disc problems or joint dysfunction. At Optimal Chiropractic, we see excellent outcomes for patients with sciatica, cervical radiculopathy, and other nerve compression issues when they fit the appropriate profile.
Go to the emergency room if you have: Loss of bowel or bladder control or numbness in the groin area. Sudden, severe symptoms following trauma. Progressive weakness that’s preventing you from walking or using your arms. Symptoms of cauda equina syndrome. Severe pain with fever, particularly if you have risk factors for infection. Symptoms following significant trauma like a car accident or major fall.
See your primary care physician when you have: Systemic symptoms like unexplained weight loss, fever, or night sweats along with nerve pain. Symptoms not clearly related to mechanical issues. A history of cancer or other serious medical conditions. Symptoms that aren’t improving after several weeks of appropriate conservative care. Concerns that warrant lab work or specialized testing.
Here in West Fargo, we encourage open communication between healthcare providers. Many of our patients at Optimal Chiropractic see us as part of a larger healthcare team. We work collaboratively with local physicians, physical therapists, and specialists to ensure everyone gets comprehensive, appropriate care. There’s no competition — just a shared goal of helping you feel better and stay healthy.
When in doubt, it’s reasonable to start with a phone call to your chiropractor or primary care physician to describe your symptoms and get guidance. Most offices are happy to help you determine the appropriate next step, even if it means directing you elsewhere for immediate care.
Symptoms Comparison Table
| Symptom Type | Simple Pinched Nerve | Serious Condition Warning Sign |
|---|---|---|
| Weakness Pattern | Mild, stable weakness in specific muscles | Progressive weakness that worsens week by week |
| Pain Location | One side of body, specific nerve distribution | Both sides of body, multiple limbs affected |
| Pain Response | Varies with position, some relief possible | Constant, severe, unrelieved by any position |
| Bladder/Bowel Function | Normal function maintained | Loss of control or difficulty emptying |
| Systemic Symptoms | None — localized to affected area | Fever, weight loss, night sweats present |
| Symptom Progression | Stable or gradually improving with care | Steadily worsening despite rest and care |
| Onset Pattern | Gradual onset related to activity/posture | Sudden onset or following significant trauma |
Myths vs. Facts About Nerve Pain
Myth: All Nerve Pain Resolves on Its Own With Time
Fact: While many cases of simple nerve compression do improve with time and appropriate care, not all nerve pain is self-limiting. Progressive conditions like worsening disc herniations, spinal stenosis, or serious underlying problems require intervention. Waiting too long with certain conditions can lead to permanent nerve damage. This is why proper evaluation is so important — to identify which cases will likely resolve conservatively and which need more aggressive intervention.
Myth: If You Can Still Move, Your Nerve Problem Isn’t Serious
Fact: Many serious nerve conditions allow for continued movement, at least initially. Early spinal cord compression, tumors, and infections may present with pain and tingling long before they cause complete loss of function. The ability to walk or use your arms doesn’t rule out a serious underlying problem. In fact, some of the most concerning conditions cause progressive symptoms — meaning function gradually declines. Don’t dismiss your symptoms simply because you’re still mobile.
Myth: Chiropractic Care Can Fix Any Type of Nerve Problem
Fact: Chiropractic care is highly effective for mechanically-based nerve compression issues, such as those caused by spinal misalignment, disc problems, or joint dysfunction. However, chiropractors recognize that not all nerve problems are within our scope of practice. Infections, tumors, cauda equina syndrome, and certain neurological diseases require medical or surgical intervention. A responsible chiropractor will screen for these conditions and refer appropriately. At Optimal Chiropractic, we pride ourselves on knowing when chiropractic care is appropriate and when other interventions are needed.
Myth: Severe Pain Always Means a Serious Problem
Fact: Pain severity doesn’t always correlate with problem severity. Some relatively straightforward disc herniations cause excruciating pain, while certain tumors may cause only mild discomfort initially. The character, pattern, and associated symptoms matter more than intensity alone. That said, severe, unrelenting pain that doesn’t respond to position changes or conservative measures does warrant investigation. The key is looking at the complete picture, not just pain level in isolation.
Myth: You Should Always Try Conservative Care First, No Matter What
Fact: While conservative care is appropriate for most musculoskeletal conditions, certain red flag symptoms require immediate medical attention before trying any conservative approach. Cauda equina syndrome, spinal infections, fractures, and other serious conditions need urgent intervention. Starting with conservative care when red flags are present can lead to delayed diagnosis and worse outcomes. This is why proper screening and evaluation are critical first steps. When red flags are absent and symptoms fit a mechanical pattern, conservative care is absolutely the right place to start.
Final Thoughts from Optimal Chiropractic
Living with nerve pain can be frustrating and frightening. Here in West Fargo, we understand that when pain shoots down your arm or leg, or when numbness starts creeping into your fingers or toes, it affects everything — your work, your sleep, your ability to enjoy time with family and friends.
The good news is that most nerve compression issues respond very well to conservative chiropractic care. We help patients every day find relief through gentle adjustments, soft tissue therapy, corrective exercises, and lifestyle modifications. These mechanical problems, while uncomfortable, rarely represent serious underlying disease.
But part of our job at Optimal Chiropractic is also recognizing when symptoms don’t fit that typical pattern. We take those five warning signs seriously because we know that early detection and appropriate referral can make all the difference when something more serious is happening. There’s no ego in healthcare — just a commitment to getting you the right care at the right time.
If you’re experiencing nerve symptoms and you’re not sure what to do next, we’re here to help. A thorough evaluation can provide clarity and direction, whether that means starting conservative chiropractic care or coordinating with other healthcare providers for additional testing. You don’t have to figure this out alone.
Your nervous system is too important to ignore or hope problems resolve on their own. Trust your instincts, pay attention to warning signs, and seek evaluation when something doesn’t feel right. The team at Optimal Chiropractic is committed to helping our West Fargo community stay healthy, active, and informed about their spine and nervous system health.
Frequently Asked Questions
How long should I wait before seeing someone about nerve pain?
For typical nerve pain without red flags, waiting a few days to a week while trying rest, ice, and gentle movement is reasonable. However, if you have any of the five warning signs mentioned in this article, seek evaluation within 24-48 hours. For loss of bowel or bladder control, go to the emergency room immediately. When in doubt, call a healthcare provider to describe your symptoms and get guidance.
Can a pinched nerve cause permanent damage?
Most pinched nerves, when addressed appropriately, don’t cause permanent damage. However, severe or prolonged nerve compression can lead to lasting problems. This is more likely with serious conditions like cauda equina syndrome, severe spinal cord compression, or untreated progressive weakness. Early intervention and appropriate care significantly reduce the risk of permanent nerve damage.
Will an X-ray show if I have a pinched nerve?
X-rays show bone structure but don’t directly visualize nerves, discs, or soft tissues. They can reveal alignment problems, arthritis, or bone spurs that might contribute to nerve compression. However, MRI is the gold standard for evaluating nerve compression, as it shows discs, nerve roots, and the spinal cord itself. Your healthcare provider will recommend appropriate imaging based on your symptoms and examination findings.
Is it safe to exercise with nerve pain?
Gentle movement is usually beneficial for simple nerve compression, but high-impact activities or movements that aggravate symptoms should be avoided. Walking, gentle stretching, and specific therapeutic exercises recommended by your chiropractor or physical therapist are typically safe and helpful. However, if you have progressive weakness or other red flag symptoms, hold off on exercise until you’ve been properly evaluated.
What’s the difference between a pinched nerve and sciatica?
Sciatica is actually a specific type of pinched nerve. It refers to compression or irritation of the sciatic nerve, which runs from your lower back down through your hips and legs. The term “sciatica” describes the location and pattern of symptoms, while “pinched nerve” is a general term for any compressed nerve. Sciatica typically causes pain that radiates from the lower back through the buttock and down the leg.
Can stress or anxiety cause nerve-like symptoms?
Stress and anxiety can cause tingling, numbness, and other sensations that mimic nerve problems, often due to muscle tension, hyperventilation, or heightened nervous system sensitivity. However, true nerve compression causes symptoms that follow specific anatomical patterns and are associated with mechanical findings on examination. Never assume symptoms are “just stress” without proper evaluation, especially if you have any red flag signs.
Key Takeaways
- Most pinched nerves respond well to conservative chiropractic care, but certain warning signs indicate something more serious that needs immediate attention
- Five critical red flags include progressive weakness, loss of bowel/bladder control, bilateral symptoms, systemic symptoms like fever or weight loss, and severe unrelenting pain
- Serious conditions like spinal cord compression, cauda equina syndrome, infections, and tumors can mimic simple pinched nerves but require urgent medical intervention
- A thorough chiropractic evaluation can help identify whether symptoms fit a mechanical pattern appropriate for conservative care or require additional medical investigation
- When red flags are present, don’t wait — seek appropriate medical attention within 24-48 hours, or immediately for loss of bowel/bladder control